Quick Actions
Contents
Mechanism of Blood Coagulation
Blood coagulation is a critical physiological process that prevents excessive bleeding after vascular injury. It involves a complex sequence of enzymatic reactions leading to the formation of a stable blood clot. Understanding the mechanism of coagulation is essential for medical laboratory science students, as it forms the basis for diagnosing bleeding disorders, monitoring anticoagulant therapy, and understanding hemostatic balance. This module explains the step-by-step mechanisms, pathways, and key factors involved in blood coagulation.
Learning Objectives
- Describe the overall process of blood coagulation and its physiological purpose.
- Identify the intrinsic, extrinsic, and common pathways of coagulation.
- Explain the role of clotting factors and their activation sequence.
- Understand the formation of fibrin and stabilization of the blood clot.
- Recognize clinical implications of coagulation defects and disorders.
- Apply correct practices in the handling and labeling of specimen containers.
Key Points to Remember
- Coagulation is the transformation of blood from a liquid to a gel to prevent blood loss.
- It involves three main pathways: intrinsic, extrinsic, and common pathways.
- Clotting factors are mostly plasma proteins, usually in inactive forms.
- Calcium ions and vitamin K are essential for several coagulation steps.
- Fibrin mesh formation stabilizes the platelet plug at the site of injury.
Introduction to Blood Coagulation Mechanism
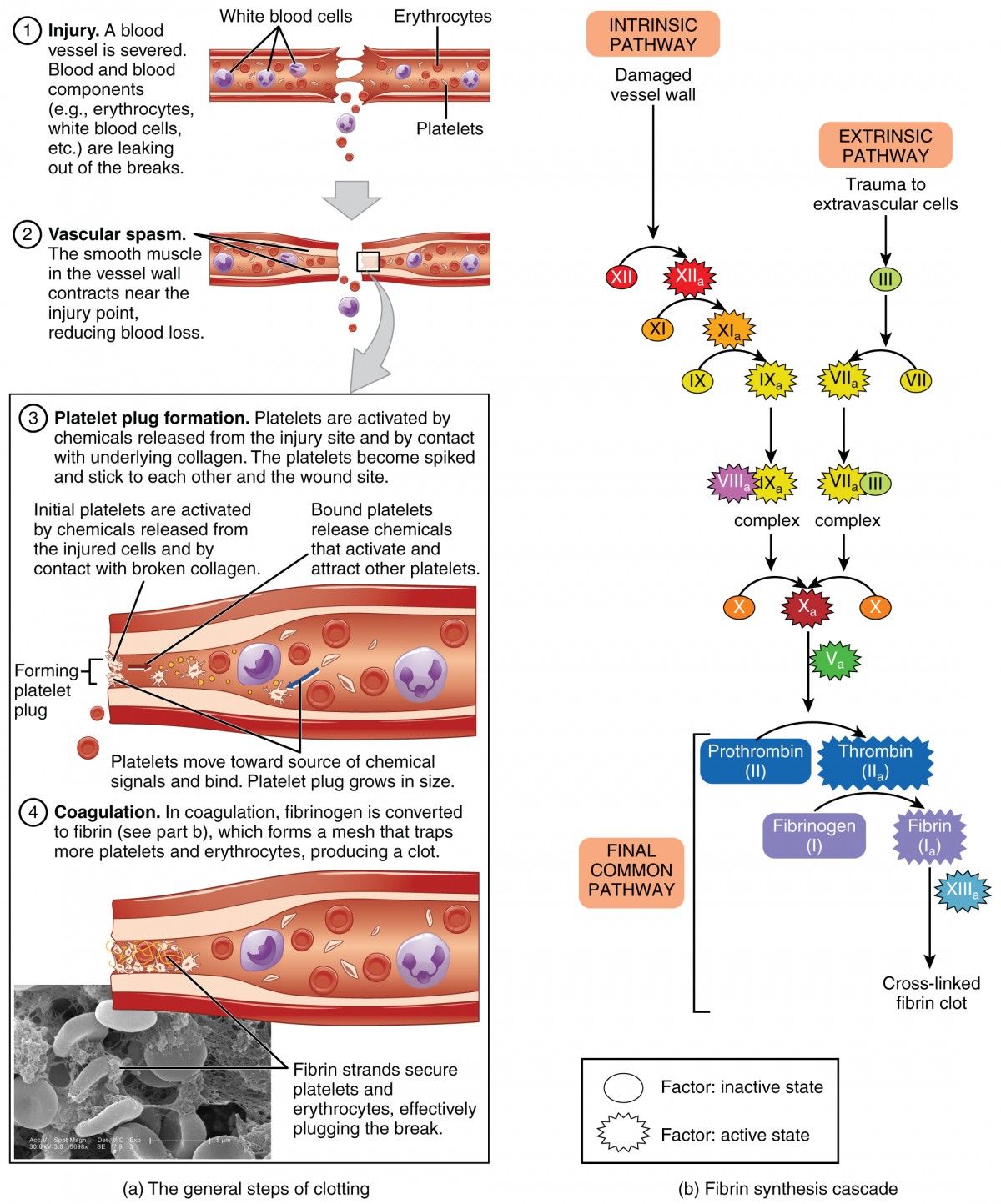
Blood coagulation is a defense mechanism that ensures hemostasis, the cessation of bleeding after vascular injury. It complements vascular spasm and platelet plug formation and leads to the creation of a stable clot that prevents further blood loss. Coagulation is tightly regulated to avoid excessive clotting or bleeding.
Coagulation Pathways
Blood coagulation occurs through three interconnected pathways:
1. Intrinsic Pathway
Triggered by damage to the endothelium or exposure of blood to negatively charged surfaces.
Involves clotting factors present within the plasma, hence intrinsic.
Key steps:
- Factor XII (Hageman factor) is activated to XIIa on contact with subendothelial collagen.
- XIIa activates Factor XI to XIa.
- XIa activates Factor IX to IXa in the presence of calcium ions.
- IXa, with Factor VIIIa, phospholipids, and calcium, activates Factor X to Xa, entering the common pathway.
Mnemonic: “TENET” — Twelve, Eleven, Nine, Eight, Ten (activation sequence to common pathway)
2. Extrinsic Pathway
Initiated by tissue injury outside the vascular system.
Involves Tissue Factor (Factor III) released by damaged tissues.
Key steps:
- Tissue factor binds Factor VII, forming TF-VIIa complex.
- The complex directly activates Factor X to Xa (common pathway).
The extrinsic pathway is faster than the intrinsic pathway, often acting as the initial response to trauma.
3. Common Pathway
Begins at Factor X activation and culminates in the formation of a stable fibrin clot.
Steps:
- Factor Xa combines with Factor Va, phospholipids, and calcium to form the prothrombinase complex.
- Prothrombinase converts prothrombin (Factor II) to thrombin (Factor IIa).
- Thrombin converts fibrinogen (Factor I) into fibrin monomers.
- Fibrin monomers polymerize to form fibrin threads, creating a soft clot.
- Factor XIIIa (activated by thrombin) cross-links fibrin, stabilizing the clot.
Role of Calcium and Vitamin K
- Calcium ions (Factor IV) are required for activation of multiple coagulation factors.
- Vitamin K is essential for the γ-carboxylation of Factors II, VII, IX, and X, enabling them to bind calcium and function properly.
Regulation of Coagulation
Coagulation is controlled to prevent unwanted thrombosis:
- Antithrombin III inhibits thrombin and Factors IXa, Xa.
- Protein C and Protein S degrade Factors Va and VIIIa.
- Tissue Factor Pathway Inhibitor (TFPI) inhibits the TF-VIIa complex.
Imbalance can result in bleeding disorders or thrombotic conditions.
Clinical Relevance
Deficiency of coagulation factors can cause hemophilia A (Factor VIII) or hemophilia B (Factor IX).
Vitamin K deficiency or anticoagulant therapy (warfarin) affects Factor II, VII, IX, X synthesis.
Laboratory tests: PT (Prothrombin Time) measures extrinsic pathway; APTT (Activated Partial Thromboplastin Time) measures intrinsic pathway.
Test Your Knowledge
Complete the quiz to check your understanding.
Ready to take the quiz?
Please log in to save your progress and see how you stack up!
Log In to ContinueAdditional Resources
See More Resourses
Watch more on YouTube
