Quick Actions
Contents
Parathyroid Hormone & Calcium Regulation
The parathyroid glands play a central role in maintaining stable calcium and phosphate levels in the body, a requirement for normal neuromuscular function, bone mineral balance, blood coagulation, and cellular signaling. Parathyroid hormone is the chief regulator of extracellular calcium, acting rapidly on bone, kidneys, and indirectly on the intestines. This lesson explains the physiology of parathyroid hormone, the mechanisms that maintain calcium homeostasis, and the interactions between PTH, calcitonin, and vitamin D. Students will gain a comprehensive understanding of how calcium regulation supports vital biological processes and how disruptions lead to clinical disorders.
Learning Objectives
- Describe the structure and function of the parathyroid glands.
- Explain how parathyroid hormone is synthesized and secreted.
- Discuss how PTH regulates calcium and phosphate in bone, kidneys, and intestines.
- Outline the role of vitamin D in calcium absorption and its relationship with PTH.
- Identify factors that stimulate or inhibit PTH secretion.
- Explain the physiologic consequences of hypo and hyperparathyroidism.
Key Points to Remember
- PTH increases blood calcium and decreases serum phosphate.
- Calcium sensing receptors on parathyroid cells regulate PTH release.
- PTH stimulates bone resorption, renal calcium reabsorption, and vitamin D activation.
- Active vitamin D enhances intestinal absorption of calcium.
- Calcitonin opposes PTH but has a minor role in humans.
Anatomy and Structure of the Parathyroid Glands
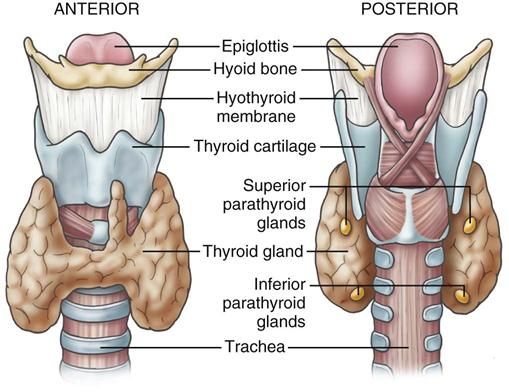
The parathyroid glands are small, oval endocrine glands located on the posterior surface of the thyroid gland. Most individuals have four glands, though the number may vary. They are composed mainly of chief cells, which produce parathyroid hormone, and oxyphil cells whose function is less defined.
Chief Cells
Chief cells monitor circulating calcium levels through specialized calcium sensing receptors. When calcium falls, these receptors trigger increased PTH release.
Oxyphil Cells
Oxyphil cells are larger and more eosinophilic. Their exact function is uncertain, but their numbers increase with age.
Parathyroid Hormone: Synthesis and Secretion
PTH is synthesized as prepro PTH, processed to pro PTH, and finally to active PTH containing 84 amino acids. It is stored in secretory granules until needed.
Control of PTH Secretion
PTH secretion is regulated primarily by extracellular calcium concentration.
Key mechanism:
Low calcium activates PTH release.
High calcium inhibits PTH release.
The calcium sensing receptor on chief cells detects changes in ionized calcium and adjusts hormone secretion instantly.
Other Regulators
A useful memory aid for PTH stimulators is L P M
PTH Actions on Bone
PTH acts on bone to increase calcium and phosphate release.
Mechanism
PTH does not act directly on osteoclasts. Instead, it binds to receptors on osteoblasts, which then release signals that activate osteoclasts. Osteoclasts break down bone matrix, releasing calcium and phosphate into the bloodstream.
Intermittent vs Continuous PTH
PTH Actions on the Kidneys
The kidneys are essential targets for PTH in calcium regulation.
Effects on Calcium
Effects on Phosphate
Mnemonic:
PTH = “Phosphate Trash Hormone” because it reduces phosphate reabsorption.
Activation of Vitamin D
PTH stimulates 1-alpha hydroxylase in the kidneys, converting inactive vitamin D into active calcitriol. Calcitriol increases calcium absorption from the intestine.
PTH Effects on the Gastrointestinal Tract
PTH does not directly act on the intestines, but it increases calcium absorption indirectly.
Mechanism
Vitamin D and Calcium Regulation
Vitamin D complements PTH in maintaining calcium balance.
Sources of Vitamin D
Activation Pathway
- Vitamin D3 enters circulation.
- Converted to 25 hydroxy vitamin D in the liver.
- Converted to active 1,25 dihydroxy vitamin D in the kidneys through PTH stimulation.
Functions of Active Vitamin D
Calcitonin: The Opposing Hormone
Calcitonin, produced by parafollicular C cells in the thyroid, lowers blood calcium by inhibiting osteoclast activity. However, its role in humans is limited compared to PTH.
Actions of Calcitonin
Calcitonin is more important in childhood and pregnancy when bone turnover is rapid.
Calcium and Phosphate Balance
Calcium and phosphate regulation are linked through PTH and vitamin D.
Calcium Functions
Phosphate Functions
PTH maintains a balance by increasing calcium levels while reducing phosphate levels.
States of Calcium Balance
Positive Calcium Balance
Occurs during growth, pregnancy, or bone healing when intake exceeds loss.
Negative Calcium Balance
Seen in vitamin D deficiency, chronic kidney disease, or postmenopausal bone loss.
Disorders of Parathyroid Function
Hyperparathyroidism
Overproduction of PTH causes hypercalcemia.
Primary Hyperparathyroidism
Secondary Hyperparathyroidism
Symptoms of Hypercalcemia
Hypoparathyroidism
Insufficient PTH causes hypocalcemia.
Causes
Symptoms of Hypocalcemia
Test Your Knowledge
Complete the quiz to check your understanding.
Ready to take the quiz?
Please log in to save your progress and see how you stack up!
Log In to ContinueAdditional Resources
See More Resourses
Watch more on Youtube
